Can a vasectomy be reversed? Vasectomy reversal success rates and more

Vasectomy reversal is an option, but it’s not guaranteed to recover fertility. Let’s explore the vasectomy reversal procedure, vasectomy reversal success rates, and more.
Are vasectomies 100% reversal? Vasectomy, a surgical procedure for male birth control, should be considered permanent. Vasectomy reversal is an option, but it’s not guaranteed to recover fertility. Let’s explore the vasectomy reversal procedure, vasectomy reversal success rates, and more.
Key takeaways
- For those who change their mind about their vasectomy, vasectomy reversal surgery may be an option.
- There is no guarantee that a vasectomy reversal will return your fertility to your pre-vasectomy level. Factors affecting vasectomy reversal success rates include how long it has been since the initial vasectomy, how the initial procedure healed, and even the expertise of the surgeon performing the vasectomy reversal.
- Vasectomy reversals are expensive, invasive, and require long recovery periods.
- Sperm freezing before vasectomy may help you avoid vasectomy regret, and give you options for growing your family in the future without a vasectomy reversal.
Vasectomy reversal procedure
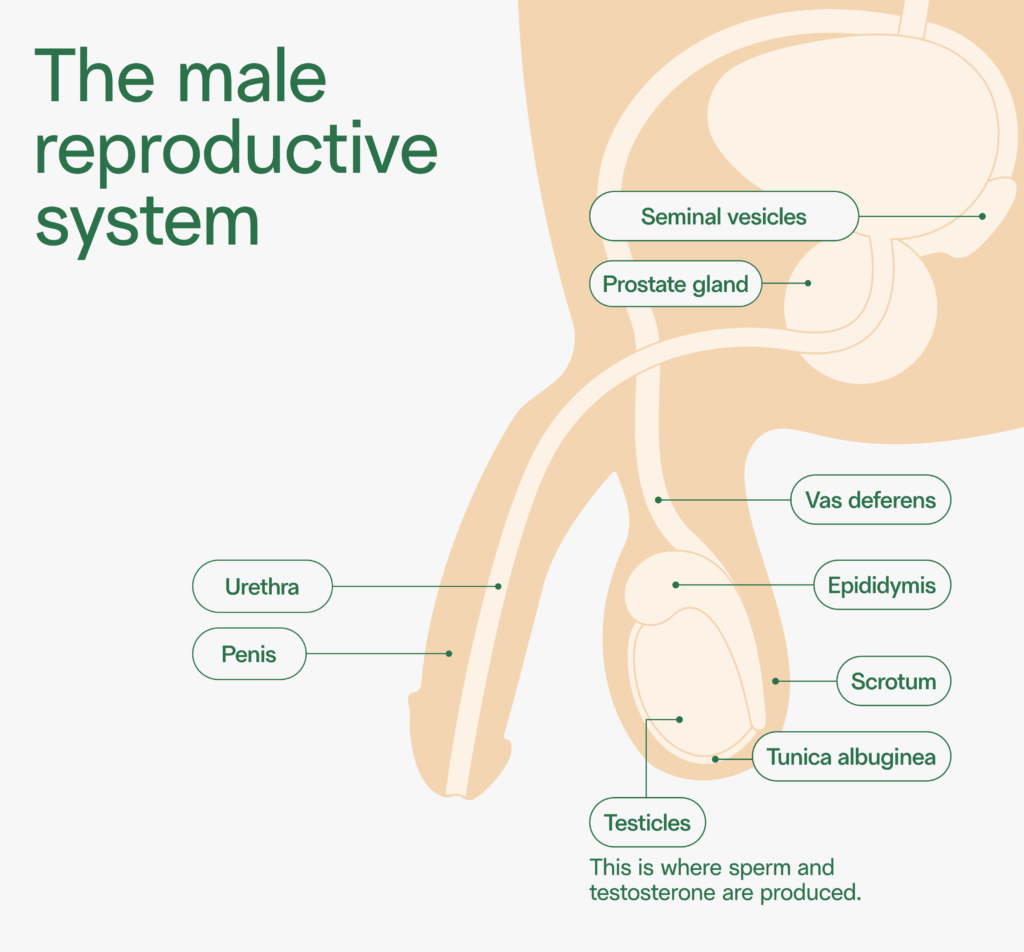
To understand vasectomy reversal, it’s first helpful to know how a vasectomy works. Typically performed by a urologist, vasectomy is a fairly straightforward procedure. It’s an outpatient surgery with local anesthesia. The doctor will make a small incision or puncture before snipping the vas deferens (the tubes that carry sperm out of the testes) on each side, and then seal everything up. A vasectomy usually takes less than 30 minutes, and requires only a few days’ recovery.
Many people mistakenly believe that vasectomies can be reversed just as simple. However, vasovasostomy, the technical term for vasectomy reversal, is a technically demanding procedure.
During a vasectomy reversal, a surgeon will attempt to reconnect the vas deferens to allow sperm to leave the body once again. Vasectomy reversal requires general anesthesia, and takes several hours in the operating room.
You can’t get a vasectomy reversal without surgery. In fact, vasectomy reversal is a type of microsurgery, a more complex procedure that uses tiny, precise tools and is completed under magnification with a microscope.
Legacy’s Director of Clinical Services, Stephanie Sabourin, has been involved in over 2,000 vasectomies. “Think about trying to operate on a cooked piece of angel hair pasta with a hollow center, and you need to precisely realign it. That’s pretty much what a vasectomy reversal is like,” Stephanie says. “This is a really complex and delicate procedure.”
Vasectomy reversal specialist
As with a vasectomy, the specialist that performs vasectomy reversal is a urologist. Urologists are experts in the uro-genital system, including the:
- Bladder
- Kidneys
- Urethra
- Testicles
- Penis
- Seminal vesicles
- Prostate
- Vas deferens
However, while the majority of urologists perform vasectomy, not every urologist has experience with the microsurgical techniques involved with vasectomy reversal. A 2004 survey found that less than half of urologists who responded performed vasectomy reversals as part of their practice.1
Research has found that the experience of your doctor has a significant impact on success rates after a vasectomy reversal.2,3,4 One study found that specialists who perform vasectomy reversals more often have 36% higher success rates than general surgeons. If you’re considering a specialist for vasectomy reversal, look for an experienced surgeon who does reversals regularly.
Vasovasostomy vs. vasoepididymostomy
The vasectomy reversal procedure will vary slightly depending on which of the two methods — vasovasostomy or vasoepididymostomy — your surgeon uses.
Vasovasostomy (VV) is a vasectomy reversal in which the surgeon reconnects the cut ends of the vas deferens. This is the more common of the two vasectomy reversal procedures.
Vasoepididymostomy (VE) is a more complex procedure in which the surgeon connects the vas deferens directly to the epididymis, the organ in the testes where sperm are stored. A urologist might choose VE vs. VV if there appears to be a blockage in the epididymis or vas deferens as a result of the original vasectomy.
A blockage can only be discovered during surgery. Therefore, there is no way to know in advance which of the two vasectomy reversal methods your doctor will use. Sometimes, a surgeon may have to use both techniques — a vasovasostomy on one side, and a vasoepididymostomy on the other.
Vasectomy reversal recovery
How painful is a reverse vasectomy? Most men report that a vasectomy reversal involves more pain than the initial vasectomy. Groin and testicular pain for 1–3 weeks is considered normal.
After a vasectomy reversal, many men take 3–5 days off of work to recover at home. Most experts recommend avoiding strenuous exercise and heavy lifting for 4–8 weeks, and no masturbation or sex for 2–4 weeks after a vasectomy reversal.
Vasectomy reversal recovery generally involves:
- Wearing tight, supportive undergarments for the first few weeks, to reduce movement of the testicles.
- Icing the area for several days.
- Limiting exercise for up to 8 weeks after the surgery.
- Refraining from ejaculation for at least 2 weeks.
Vasectomy reversal success rates
When it comes to vasectomy reversal there are two different measurements of success:
- Patency rate, the percentage of vasectomy reversals that are able to re-establish the flow of sperm out of the body.
- Clinical pregnancy rate or live birth rate, the percentage of vasectomy reversals that result in a pregnancy or a baby, respectively.
Patency rates after vasectomy reversal
Patency can be determined with a semen analysis. Vasectomy reversal patency rates vary widely based on a number of factors, including:
- How long it has been since the original vasectomy
- The experience of the surgeon
- The presence of any blockages or scarring as a result of the initial vasectomy
- Whether the surgeon performed a vasovasostomy or vasoepididymostomy
Source: Amarin et al, 2005.
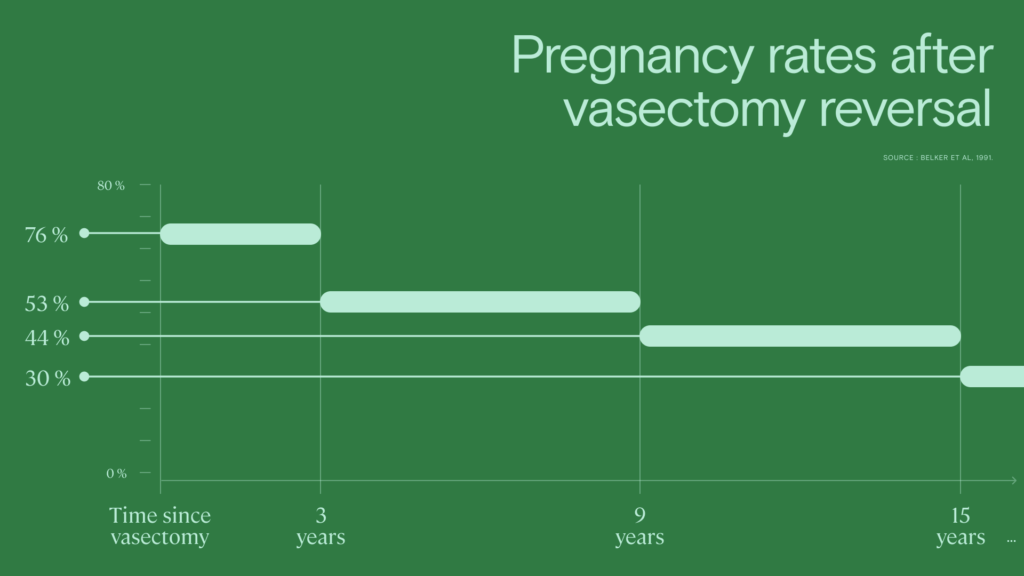
Pregnancy rates after vasectomy reversal
Not every vasectomy reversal that achieves patency will achieve pregnancy. Pregnancy rates after vasectomy reversal can be as low as 30%.
A few factors can influence the chances of pregnancy after a vasectomy reversal:
- How long it has been since the original vasectomy
- The experience of the surgeon
- The presence of any blockages or scarring as a result of the initial vasectomy
- Whether the surgeon performed a vasovasostomy or vasoepididymostomy
- Baseline sperm health prior to vasectomy
- Medical history, such as a history of smoking
- The age of both partners
- The results of any female fertility testing
How vasectomy and vasectomy reversal impact fertility
Why are pregnancy rates so much lower than patency rates?
While many believe their sperm will be just as healthy after vasectomy reversal as it was before the original vasectomy, the truth is that testicular surgery can damage sperm health long-term. After a vasectomy reversal, men may experience:
- Lower sperm count
- Lower motility, the percentage of sperm that are moving or “swimming”
- Lower morphology, the percentage of sperm that are the proper shape
- Higher sperm DNA fragmentation, the percentage of sperm that contain damaged DNA
A study from 1990 found that, after a vasectomy reversal, patients experienced “characteristic defects occur in sperm motility, sperm membrane function and morphology.”7 While vasectomy reversal technology has advanced since then, more recent studies have similar findings.
A 2005 study looked at sperm extracted directly from the testes in men who had a vasectomy.8 The study found that sperm production was actually lower — by about 40% — than sperm production in non-vasectomized men. A 2021 review concluded that, for men who have had a vasectomy reversal, “sperm motility and number were decreased, sperm DNA fragmentation was increased, sperm production was inhibited… and abnormal sperm formation [was] induced.”9 In other words, every sperm parameter was poorer after vasectomy reversal than before.
This is likely due to trauma, scarring, and inflammation in the testes as a result of both the initial vasectomy and the reversal surgery. Surgery to the testes can also introduce antisperm antibodies, immune system proteins that mistakenly destroy sperm. Multiple studies have found that antisperm antibodies are present in the semen of over half of men who have had a vasectomy reversal.7,10,11
How do I know my vasectomy reversal worked?
The best way to understand if your vasectomy reversal worked is to get a semen analysis. This is a laboratory test in which a lab scientist examines your semen sample under a microscope. A semen analysis after vasectomy reversal can determine not only if sperm are present — in other words, if you have achieved patency — but also measure the count, motility, and morphology of the sample.
Men who have had a vasectomy should test their sperm multiple times in order to monitor how their sperm quality is recovering. They should also consider getting advanced sperm testing such as DNA fragmentation analysis, since vasectomy reversal is known to increase damage to sperm’s DNA.
How long does it take to get pregnant after a vasectomy reversal?
Pregnancy after a vasectomy reversal is not guaranteed, and it’s difficult to give a timeline. It may take 6–12 months or more for sperm quality to recover after a vasectomy, if it does. One small study found that the average time to pregnancy after vasectomy reversal was 16.3 months.12
Cost of vasectomy reversal
Due to the necessity of general anesthetic and the time the procedure takes, vasectomy reversal costs are much higher than the cost of the original vasectomy.
Typically, a vasectomy reversal costs between $5,000 and $15,000. If your surgeon discovers a blockage and you require a more complex surgery, this price could increase further.
Is vasectomy reversal covered by insurance?
Not usually. Vasectomy reversal is considered an elective procedure and is not typically covered by health insurance.
Avoid vasectomy reversal by freezing sperm before vasectomy
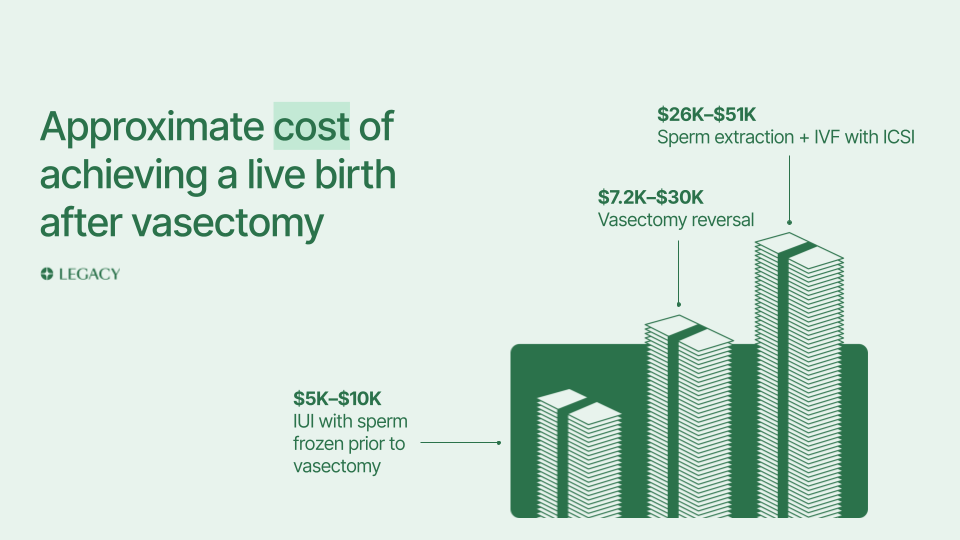
Up to 10% of men will eventually regret their vasectomy and seek a vasectomy reversal. If you have not yet undergone a vasectomy, freezing sperm beforehand is the best possible way to protect yourself against vasectomy regret.
Freezing sperm is non-invasive, requiring a few semen samples collected via masturbation before your vasectomy. Frozen sperm can be used in several fertility procedures in the future. Using frozen sperm for IUI or IVF after a vasectomy is more affordable, less painful, and potentially more effective than attempting a vasectomy reversal. (Plus, you won’t need to get another vasectomy afterward.)
Learn more about freezing sperm before your vasectomy.
References
- Crain et al, “Practice patterns in vasectomy reversal surgery: results of a questionnaire study among practicing urologists.” 2004.
- Hertz et al, “Impact of surgical volume and resident involvement on patency rates after vasectomy reversal—A 14-year experience in an open access system.” 2021.
- Wood et al, “Current practice in the management of vasectomy reversal and unobstructive azoospermia in Merseyside & North Wales: a questionnaire-based survey.” 2003.
- Patel et al, “Vasectomy reversal: a clinical update.” 2016.
- Amarin et al, “Patency following vasectomy reversal. Temporal and immunological considerations.” 2005.
- Gerrard et al, “Effect of female partner age on pregnancy rates after vasectomy reversal.” 2007.
- Urry et al, “A fifteen-year study of alterations in semen quality occurring after vasectomy reversal.” 1990.
- McVicar et al, “Effects of vasectomy on spermatogenesis and fertility outcome after testicular sperm extraction combined with ICSI.” 2005.
- Yang et al, “Review of Vasectomy Complications and Safety Concerns.” 2021.
- Wegmann et al, “Vasectomy, anti-sperm antibodies and arterial damage.” 1980.
- Marks et al, “Antisperm antibodies: prevalance, patterns and impact on natural conception following vasectomy reversal.” 2013.
- Valerie et al, “Pregnancy after vasectomy: surgical reversal or assisted reproduction?” 2018.
Find what's right for you


