Vasectomy myths and misconceptions

Vasectomy is a common birth control procedure, but many vasectomy myths and misconceptions that surround the process. In this article, we explore the truth about getting “the snip.”
Vasectomy is a common birth control procedure, performed roughly half a million times yearly. Nonetheless, there are many vasectomy myths and misconceptions that surround the process. In this article, we will explore some of those incorrect assumptions and highlight the truth about getting “the snip.”
Key takeaways
- There are a number of vasectomy myths that may stop men from seeking the procedure, even if it’s right for them — or may prevent vasectomy patients from taking steps to prevent regret.
- Having a vasectomy will not lower your testosterone, change your libido or affect your sexual function or your sexual satisfaction. Most people have better sex after the procedure.
- Vasectomies are not always easily reversible and should be considered a permanent procedure. If there’s a chance you might want kids in the future, you should consider sperm freezing before your vasectomy.
- Vasectomies do not take effect immediately, and you should confirm sterilization with a post-vasectomy semen analysis before stopping other forms of contraception.
Vasectomy myths are commonplace
A vasectomy is a medical procedure performed as a form of permanent birth control.
There is a wealth of misinformation currently circulating when it comes to men’s health, as evidenced by a 2022 study looking at the inaccuracies of advice around testosterone, semen retention, and vasectomy on TikTok and Instagram.1
Legacy’s Sperm Report, a survey of almost 3,000 Americans published in 2023, had similar findings. Over 1/3 of respondents believed that vasectomy reversals were guaranteed to restore fertility. (In reality, pregnancy rates after vasectomy reversal can be as low as 30% — more on that below.)
When it comes to male contraception, there are very few choices. Vasectomy is the only long-term birth control option for men. Let’s clear up any misconceptions around vasectomy so that men can make informed choices about whether to have a vasectomy, or not.
Myth: Getting a vasectomy will lower your testosterone levels.
Truth: Testosterone levels are not affected by vasectomy.
Many men are concerned that having a vasectomy will affect their testosterone levels, but this is not the case. A 2018 study showed that vasectomy had no impact on the long-term levels of sexual hormones in men.2
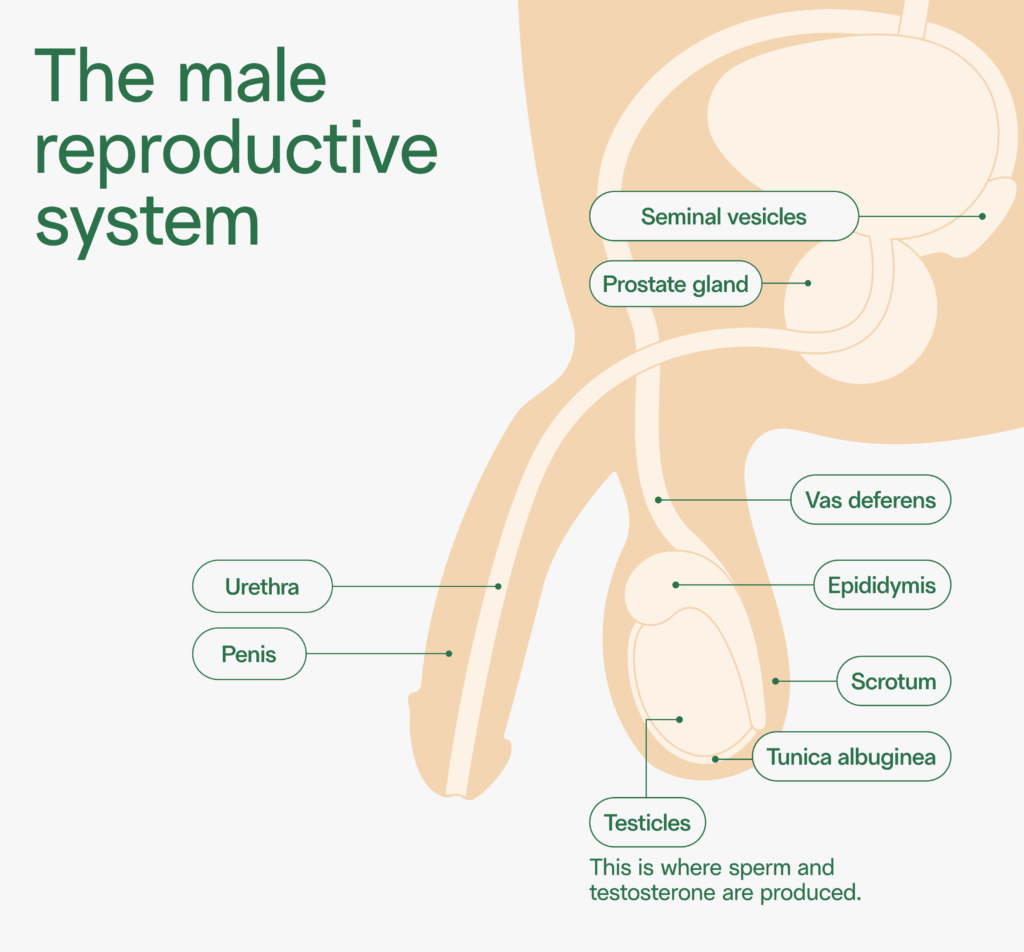
Testosterone is produced in the testes, which remain intact after a vasectomy. Vasectomy is a short 10–15 minute procedure in which the vas deferens, the tube that carries the semen from the testicle, is cut and sealed. The procedure stops the sperm from entering the semen, but it does not affect the body’s ability to make testosterone.
Learn more about how a vasectomy will affect your hormones.
Myth: Vasectomies change sexual function or libido.
Truth: Everything down there will work the same — and you may even have more sex.
Testosterone is the main hormone responsible for sex drive or libido. As discussed, vasectomy will not affect testosterone, and therefore will not affect your sex drive.
Men who have undergone a vasectomy can rest assured that they will still ejaculate semen as before, but the semen will not contain sperm. (Since sperm is only 2–5% of semen, there’s no noticeable impact on semen volume.) For all intents and purposes, sex post-vasectomy should be exactly the same as it was prior.
Vasectomy does not cause erectile dysfunction or any other form of sexual dysfunction. In fact, doctors and patients alike report that having a vasectomy may lead to increased sex frequency and satisfaction, as the fear of unintended pregnancy is removed from the equation.
A study carried out in 2017 looked at the impact of vasectomy on sexual satisfaction in couples. They found that sexual satisfaction improved for sterilized men, and the satisfaction of the female partner was not affected at all by the vasectomy.3
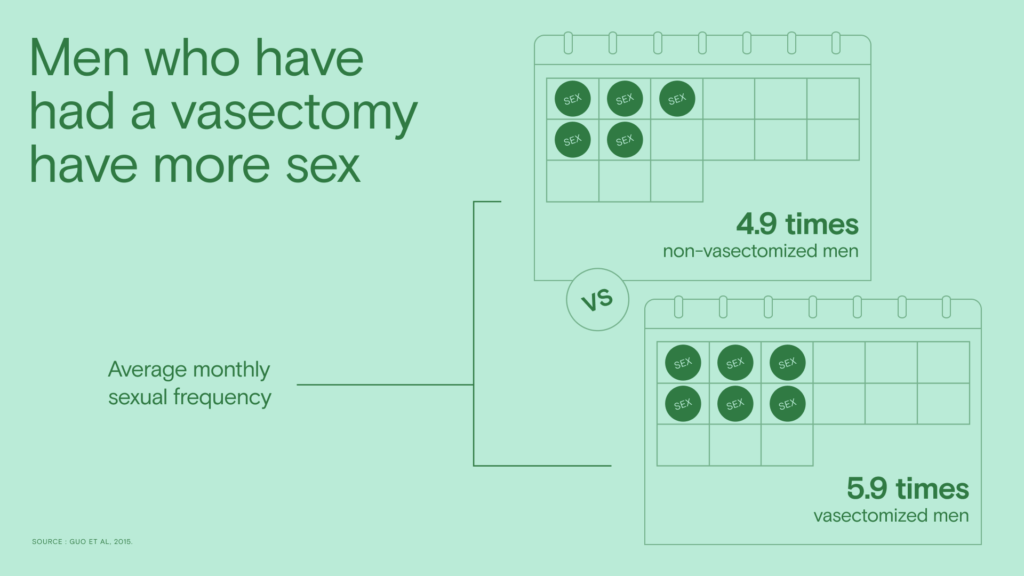
Another study found that vasectomized men are having sex, on average, 6 times per month, while non-vasectomized men are having sex 5 times per month. The same study calculated that “after adjusting for age, marital status, race, education, health, body mass index, children, and income, vasectomized men had an 81% higher odds… of having intercourse at least once a week compared with non-vasectomized men.”4
A recent review made similar conclusions, finding that showed that, following a vasectomy, men and their female partners report:
- Improved erectile function.
- Improved orgasms.
- Increased libido.
- More instances of sexual contact per month.5
Myth: Vasectomy is easily reversible.
Truth: Vasectomy reversal is expensive, invasive, and has no guarantee of success.
A study in 2013 found that as many as 20% of men later regret their decision for sterilization.6 This regret has been linked with the high rate of divorces and separation, which leads men to find new partners who then want children with them. About 2% of men end up going through a vasectomy reversal procedure within ten years of their original vasectomy.
The most common vasectomy myth is that the procedure is easily reversible if a man changes his mind. This is perpetuated in pop culture conversations around vasectomy. In reality, vasectomy reversal is much more complex than the original procedure, and many factors may contribute to low success rates after a vasectomy reversal.
The process for reversal involves a surgeon reconnecting the previously sealed vas deferens tube to your testicles, so that you can potentially ejaculate sperm once again. These tubes are tiny, and may be difficult to reconnect thanks to scar tissue. As a result of the complexity of a vasectomy reversal, it’s much longer than the original vasectomy, and requires general anesthetic as opposed to local.
As you might imagine, this also means that the cost will be significantly higher. Vasectomy reversal is typically not covered by health insurance.
Finally, there is no guarantee that a vasectomy reversal will be successful. Pregnancy rates could be as low as 30% after a reversal, and vary depending on how long ago the original vasectomy was done, how it healed, and even the expertise of the surgeon.
If you’d like to get a vasectomy with a plan B, sperm freezing is the ideal solution. Learn more about sperm freezing before a vasectomy.
Myth: Vasectomies are immediately effective.
Truth: Sperm can remain in semen for several months after vasectomy.
Most men are well enough to resume sexual intercourse within a week of their surgery. However, you will need to continue to use other forms of birth control, such as condoms. This is because some sperm will remain in the tubes leading to the penis following a vasectomy, until it’s “flushed out” with regular ejaculation.
You should not consider yourself to be sterile until you have submitted 1–2 semen samples for analysis and gotten the all-clear — no sperm remaining in the semen. Vasectomies are more than 99% effective, but the small number of pregnancies following vasectomy are typically a result of having unprotected sex too soon.
Legacy makes it easy to check the results of your vasectomy with at-home semen analysis.
References
- Dubin et al, “The broad reach and inaccuracy of men’s health information on social media: analysis of TikTok and Instagram.” 2022.
- Zhao et al, “Long-term safety, health and mental status in men with vasectomy.” 2018.
- Engl et al, “Impact of vasectomy on the sexual satisfaction of couples: experience from a specialized clinic.” 2017.
- Guo et al, “Relationship between Vasectomy and Sexual Frequency.” 2015.
- Yang et al, “Vasectomy and male sexual dysfunction risk.” 2020.
- Sharma et al, “Vasectomy demographics and postvasectomy desire for future children: results from a contemporary national survey.” 2013.
Find what's right for you


